3D mammography/tomosynthesis: Imaging with more clarity for better cancer detection
It’s a piece of equipment that gives women a significantly better chance of detecting breast cancer: the 3D mammogram or digital breast tomosynthesis.
According to a large Swedish study, the Malmo study involving 15000 women screened over a 5 year period, and using the same tomosynthesis machines as those at Mercy Radiology, it was found that breast tomosynthesis detected over a third more breast cancers (34%) than traditional 2D mammography.
The difference between the 2D technology and the 3D mammography is compelling, says Dr Sugania Reddy, lead radiologist for breast imaging at Mercy Radiology. The 2D mammogram typically produces four images (two for each breast). Tomosynthesis produces multiple images of the breast depending on the size of the breast(somewhere between 60-80 images), scanning at a much more detailed level to build up 3D representations. While 2D mammograms still find many breast cancers, using tomosynthesis over the last few years at Mercy Radiology has allowed us to detect some breast cancers that could only be seen only 3D tomosynthesis.
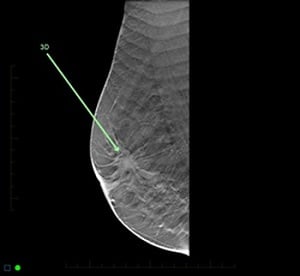
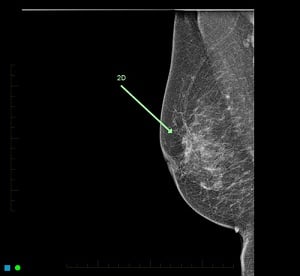
A breast cancer clearly detected on tomosynthesis (3D) and poorly on the 2D mammogram
“There’s another big difference,” says Reddy, “in that the 2D images are prone to overlapping of a breast cancer by normal breast tissue. On a 2D mammogram, the fatty tissue of the breast appears dark and fibro-glandular tissue appears as white. Unfortunately, most cancers are also white and occur in the white fibro-glandular tissue – meaning they are much harder to detect. Tomosynthesis prevents this overlap so that the cancer can be seen separately from the normal breast tissue.
A further benefit is that 3D technology also reduces patients’ recall rates. 2D technology can sometimes cause overlapping normal breast tissue on the mammogram to look like a cancer. This is reduced with tomosynthesis and therefore simply causes much less anxiety by preventing recalling a patient for extra views to confirm overlap of normal breast tissue.
Watch video here
For more information, please visit website of Breast Cancer Foundation.